Breast cancer is now the most diagnosed cancer and the leading cause of death among women.[1] According to the World Health Organization and the World Cancer Research Fund, breast cancer is the world’s second most common form of cancer; in 2020, an estimated 2.3 million new cases were diagnosed, and 685,000 lives were lost globally. This #BreastCancerAwareness Month, we hope to do our part and continue to throw light on the enormity of this disease.
With breast cancer mortality statistics, it is clear that early detection impacts a patient’s overall survival, i.e., 99% relative five-year survival rates for localized breast cancer versus 27% when metastatic.[2] This means if the cancer is caught early when it is still localized, there’s an almost 100% chance of survival versus after it has spread.
Are We Doing Enough to Address Breast Cancer Care?
Globally, breast cancer screening is a proven, aggressive, and cost-effective strategy to reduce mortality and lower the associated healthcare costs. In the past several decades, international campaigns, nationwide programs and worldwide initiatives have immensely helped increase public awareness about the disease and subsequent screening rates, helping reduce mortality rates, which still hover around 30% globally.[3] Population-based screening programs (once every two or three years) have been initiated by countries for more than two decades to aid in early diagnosis, resulting in an estimated 100 million-120 million mammography procedures worldwide.
Breast Cancer and Screening Statistics Overview, 2021, Global
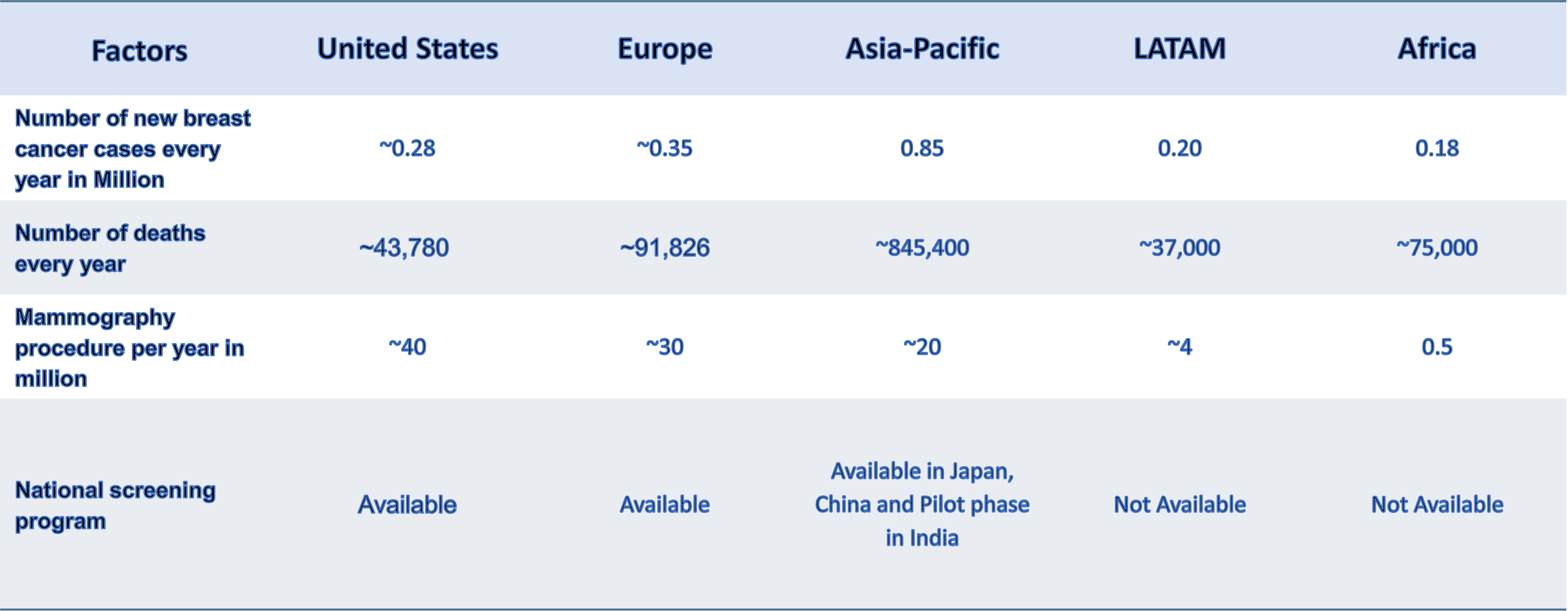
Challenges Associated with Current Cancer Screening Protocols and Role of Technologies in Early Cancer Detection
Still, with mammography as the current gold standard and ultrasound as a supplemental screening tool for cancer diagnosis, radiologists reportedly miss up to 30% of cancers. Moreover, about 80% of women recalled for follow-up testing have normal outcomes, with breast biopsies proving benign in up to 40% of cases.[4] This points to inefficiencies in our current system and approach. Hence, screening strategies that weed out inefficiencies, and do not miss or misinterpret tumors and micro-calcifications, are therefore critical.
Additionally, patient-associated barriers to continued surveillance remain, impacting efforts to cure breast cancer. For instance, breast compression, necessary in conventional mammography, is painful for some women, leading to up to 50% of women potentially skipping regularly recommended screenings due to pain and discomfort.[5]
Looking Ahead
Promising technologies like automated breast ultrasound and advanced breast computed tomography will address patient compliance and encourage regular screening. Government-funded research to assess the use of artificial intelligence technologies for the accurate detection of breast cancer tissues and further integrate the solutions into national screening programs in the coming years is expected to enhance early detection.
Thus, the role of regulatory bodies, non-governmental organization (NGO) campaign programs, patient compliance, as well as investments from public and private sectors will continue to remain vital in reducing the prognosis of and mortality from breast cancer.
[1] https://www.wcrf.org/dietandcancer/cancer-trends/worldwide-cancer-data
[2] https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
[3] https://www.sciencedaily.com/releases/2019/01/190108101203.htm
[4] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5980911/
[5] https://pubmed.ncbi.nlm.nih.gov/21275649/



